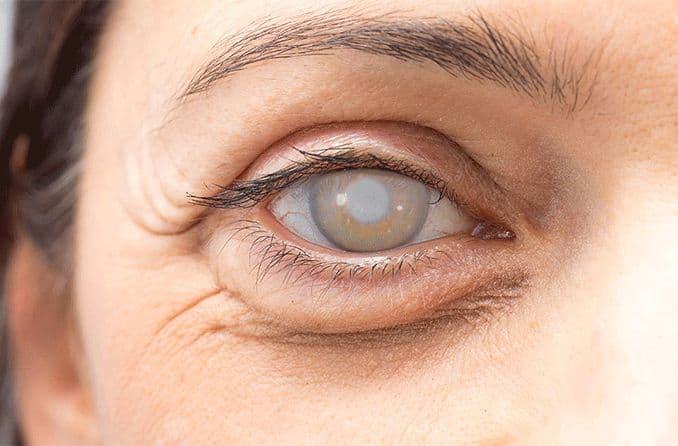
Is It Possible To Have Diabetic Retinopathy Alongside Cataracts?
For individuals living with diabetes, managing ocular health is of paramount importance. Among the ocular conditions that can arise, two commonly encountered issues are Diabetic Retinopathy and Cataracts. While these are distinct eye conditions, it is entirely possible for a person to grapple with both simultaneously. Understanding the interplay between these conditions, their respective impacts on vision, and the available treatment approaches is crucial for those navigating this dual concern. In this exploration, we delve into the intricacies of Diabetic Retinopathy and Cataracts coexistence, shedding light on how these conditions can intersect and the considerations that come into play for effective management.
Diabetic Retinopathy: Unraveling The Impact
Diabetic Retinopathy is a condition that arises due to damage to the blood vessels in the retina, the light-sensitive tissue at the back of the eye. It is a direct result of prolonged periods of high blood sugar levels, a hallmark of diabetes. Over time, the weakened blood vessels can leak or become blocked, leading to vision problems. The condition typically progresses through stages, starting with mild nonproliferative retinopathy, advancing to moderate and severe stages, and potentially culminating in proliferative retinopathy, where new blood vessels grow in the retina.
Left untreated, Diabetic Retinopathy can lead to severe vision loss or even blindness. This makes regular eye examinations crucial for individuals with diabetes. Early detection and timely intervention can significantly slow down the progression of the condition and preserve vision.
Cataracts: Clouding The Lens
Cataracts, on the other hand, affect the eye in a different way. It involves the clouding of the natural lens, which is positioned behind the iris and pupil. This clouding progressively hinders the passage of light, leading to blurry or distorted vision. Cataracts are primarily age-related but can also be influenced by other factors such as genetics or, in this context, diabetes.
For individuals with diabetes, the risk of developing cataracts is higher and they tend to develop at an earlier age. This can be attributed to the impact of prolonged exposure to high blood sugar levels, which can lead to the accumulation of excess sugar in the lens, causing it to cloud.

The Intersection: Coexistence Of Diabetic Retinopathy And Cataracts
Given the shared risk factor of diabetes, it is not uncommon for individuals to face the dual challenge of Diabetic Retinopathy and Cataracts. When these conditions coexist, the impact on vision can be substantial. The clouding of the lens due to cataracts compounds the vision problems already caused by Diabetic Retinopathy, potentially leading to more severe visual impairment.
Understanding The Risk Factors
When it comes to the coexistence of Diabetic Retinopathy and Cataracts, several risk factors may increase the likelihood of both conditions occurring simultaneously. Here are some of the key factors:
Diabetes Duration: The longer a person has been living with diabetes, the higher the risk of developing both Diabetic Retinopathy and Cataracts.
Poor Blood Sugar Control: Inadequate control of blood sugar levels over an extended period can accelerate the progression of Diabetic Retinopathy and increase the risk of developing Cataracts.
High Blood Pressure: Hypertension is a common comorbidity with diabetes. It not only exacerbates Diabetic Retinopathy but also contributes to the development of Cataracts.
Genetics and Family History: A family history of diabetes, Diabetic Retinopathy, or Cataracts can predispose an individual to an increased risk of both conditions.
Smoking and Alcohol Consumption: These lifestyle factors can worsen the progression of Diabetic Retinopathy and may also be associated with an increased risk of developing Cataracts.
Age: Both Diabetic Retinopathy and Cataracts are more common in older individuals. As age increases, so does the likelihood of developing these conditions.
Gender: Some studies suggest that there may be gender-specific differences in the risk of Diabetic Retinopathy and Cataracts. For example, in certain populations, it may be more prevalent in men.
Ethnicity: Certain ethnic groups have a higher predisposition to diabetes and its related complications, including Diabetic Retinopathy and Cataracts.
Kidney Disease: Diabetic nephropathy, or kidney disease related to diabetes, is often associated with diabetic retinopathy. It can also contribute to the development of Cataracts.
Chronic Inflammation: Conditions characterised by chronic inflammation, such as autoimmune disorders, may increase the risk of both Diabetic Retinopathy and Cataracts.
Use of Steroids: Long-term use of corticosteroids, whether orally or as eye drops, can accelerate the development of cataracts.
Other Health Conditions: Coexisting health issues like obesity, high cholesterol levels, and cardiovascular disease can contribute to the progression of both vision problems.
While these risk factors can increase the likelihood of developing both Diabetic Retinopathy and Cataracts, they do not guarantee their occurrence. Additionally, managing and controlling diabetes and its associated risk factors can help mitigate the progression of these conditions. Regular eye examinations and consultations with healthcare providers specialising in diabetes and ophthalmology are essential for early detection and effective management.

Navigating Treatment Options
Addressing both Diabetic Retinopathy and Cataracts requires a comprehensive approach. The treatment plan will be tailored to the individual's unique circumstances, considering factors such as the severity of each condition, overall health, and lifestyle.
In some cases, treatment for Diabetic Retinopathy may precede cataract surgery. This is especially true if the retinopathy is at a stage where intervention is necessary to preserve vision. Once the diabetic retinopathy is stabilised, cataract surgery can be pursued to address the clouding of the lens.
When a person has both Diabetic Retinopathy and Cataracts, it's important to consider the best approach to surgery. Here are the different types of cataract surgery available, especially for cases where Diabetic Retinopathy is a concurrent concern:
Phacoemulsification (Phaco)
This is the most common type of cataract surgery. It involves making a small incision in the cornea and using ultrasonic vibrations to break up the cloudy lens, which is then removed. This technique is often preferred because of its minimal invasiveness and rapid recovery time.
Extracapsular Cataract Extraction (ECCE)
In ECCE, a larger incision is made in the cornea, and the cataract is removed in one piece. While this technique is less common today, it may be preferred in certain cases, especially when dealing with advanced cataracts.
Manual Small-Incision Cataract Surgery (MSICS)
MSICS is similar to ECCE but involves a smaller incision. It may be used in cases where phacoemulsification is not possible or advisable.
Femtosecond Laser-Assisted Cataract Surgery (FLACS)
This technique uses a laser to assist in certain steps of cataract surgery, such as creating precise incisions and softening the cataract for easier removal. While it's not always necessary, it can offer increased precision.
Multifocal or Accommodating Intraocular Lenses (IOLs)
For individuals with both cataracts and Diabetic Retinopathy, choosing the right IOL is crucial. Multifocal or accommodating IOLs can correct vision at different distances, reducing the need for glasses after surgery.
Monofocal IOLs with Astigmatism Correction
These lenses are designed to correct astigmatism, which can be particularly important for individuals with both cataracts and Diabetic Retinopathy.
Pars Plana Vitrectomy (PPV) in Combination
In cases where advanced Diabetic Retinopathy is present, a PPV may be performed alongside cataract surgery. This procedure involves removing the vitreous gel from the eye and may be necessary to address retinal issues.
Sutureless Surgery
Modern techniques often allow for cataract surgery without the need for sutures, which can further expedite recovery.
The choice of surgery will depend on various factors, including the severity of both conditions, the patient's overall health, and the expertise of the surgeon. A thorough evaluation by an experienced ophthalmologist who is knowledgeable about both Diabetic Retinopathy and cataracts will help determine the most appropriate approach. This specialist will work in conjunction with the patient's diabetic care team to ensure comprehensive and effective management.
A Multifaceted Approach To Ocular Health
While the coexistence of Diabetic Retinopathy and Cataracts presents unique challenges, it is important to remember that effective management is indeed possible. Regular eye examinations, timely intervention, and a collaborative approach between healthcare providers specialising in diabetes, ophthalmology, and surgery can greatly improve outcomes. With advances in medical technology and a proactive stance towards ocular health, individuals facing these dual concerns can look forward to a future with a clearer vision and an enhanced quality of life.
My-iClinic's Specialised Treatment For Diabetic Retinopathy And Cataracts!
If you're facing the dual challenge of Diabetic Retinopathy and Cataracts, My-iClinic offers tailored, cutting-edge solutions designed with your unique needs in mind.
Why Choose My-iClinic For Dual Treatment?
Expertise in Diabetic Eye Care
Our experienced team understands the intricacies of managing Diabetic Retinopathy alongside Cataracts, ensuring you receive the highest standard of care.
State-of-the-Art Technology
My-iClinic employs advanced techniques, including the latest in laser and surgical interventions, to provide you with the best possible outcomes when you visit the eye clinic in London.
Personalised Approach
We believe in individualised care. Your treatment plan will be carefully crafted to address your specific conditions, ensuring optimal results.
Comprehensive Follow-Up Care
Our commitment to your well-being extends beyond the procedure. We'll be with you every step of the way, monitoring your progress and addressing any concerns.
Don't Let Diabetic Eye Conditions Hold You Back. Take the First Step Towards Clearer Vision Today!
Contact My-iClinic or schedule your consultation. Together, let's embark on a journey to a better vision and a brighter future.
Find out more by Speaking to our team